Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
What Is Gout?
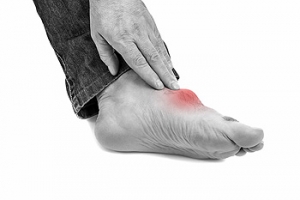
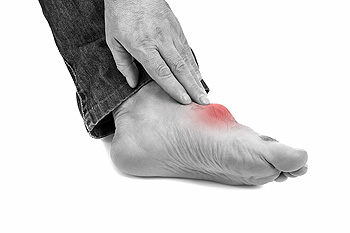 Gout is a form of inflammatory arthritis that impacts one joint at a time, usually the big toe joint, lesser toe joints, the ankle, and/or the knee. This type of arthritis is caused by a condition called hyperuricemia, where too much uric acid in the body leads to the build-up of uric acid crystals in joints, fluids, and tissues in the body. Hyperuricemia is more apt to develop in males, those who are obese, those with health conditions – such as congestive heart failure, high blood pressure, or diabetes – and those taking certain medications, like diuretics. Gout does not always develop from hyperuricemia, but if it does, it can flare up and be intensely painful (with swelling and redness). An episode of gout can have a sudden onset and last from days to weeks. Though there is no cure for gout, it can be treated and managed with proper care. If gout is suspected in the toes, a podiatrist can perform tests to confirm the diagnosis, treat it (often with medication) and help manage future bouts of the condition.
Gout is a form of inflammatory arthritis that impacts one joint at a time, usually the big toe joint, lesser toe joints, the ankle, and/or the knee. This type of arthritis is caused by a condition called hyperuricemia, where too much uric acid in the body leads to the build-up of uric acid crystals in joints, fluids, and tissues in the body. Hyperuricemia is more apt to develop in males, those who are obese, those with health conditions – such as congestive heart failure, high blood pressure, or diabetes – and those taking certain medications, like diuretics. Gout does not always develop from hyperuricemia, but if it does, it can flare up and be intensely painful (with swelling and redness). An episode of gout can have a sudden onset and last from days to weeks. Though there is no cure for gout, it can be treated and managed with proper care. If gout is suspected in the toes, a podiatrist can perform tests to confirm the diagnosis, treat it (often with medication) and help manage future bouts of the condition.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Joe Mathew George DPM, FACFAS from Illinois. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact our offices located in Joliet, Bolingbrook, and Channahon, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Everything You Need to Know About Gout
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
What are Achilles Tendon Injuries
The Achilles tendon is the strongest tendon in the human body. Its purpose is to connect the lower leg muscles and calf to the heel of the foot. This tendon is responsible for facilitating all types of movement, like walking and running. This tendon provides an enormous amount of mobility for the body. Any injuries inflicted to this tissue should be immediately brought up with a physician to prevent further damage.
The most common injuries that can trouble the Achilles tendon are tendon ruptures and Achilles tendinitis. Achilles tendinitis is the milder of the two injuries. It can be recognized by the following symptoms: inflammation, dull-to-severe pain, increased blood flow to the tendon, thickening of the tendon, and slower movement time. Tendinitis can be treated via several methods and is often diagnosed by an MRI.
An Achilles tendon rupture is trickier to heal, and is by far the most painful injury. It is caused by the tendon ripping or completely snapping. The results are immediate and absolutely devastating, and will render the patient immobile. If a rupture or tear occurs, operative and non-operative methods are available. Once the treatment begins, depending on the severity of the injury, recovery time for these types of issues can take up to a year.
Simple preventative measures can be taken as a means to avoid both injuries. Prior to any movement, taking a few minutes to stretch out the tendon is a great way to stimulate the tissue. Calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses are all suggested ways to help strengthen the lower legs and promote Achilles tendon health.
Many problems arise among athletes and people who overexert themselves while exercising. Problems can also happen among those who do not warm up properly before beginning an activity. Proper, comfortable shoes that fit correctly can also decrease tendon injuries. Some professionals also suggest that when exercising, you should make sure that the floor you are on is cushioned or has a mat. This will relieve pressure on the heels. A healthy diet will also increase tendon health.
It is very important to seek out a podiatrist if you believe you have an injury in the Achilles region. Further damage could result in severe complications that would make being mobile difficult, if not impossible.
How to Know if Your Ankle Is Broken
 If you sustain an injury to your ankle and wonder whether it is broken or not, you should remain calm and assess your symptoms. A broken ankle is quite painful, especially when you try to move it or put weight on it. The ankle is usually swollen from blood or fluid accumulating at the site of injury and it may be discolored or bruised. Less common symptoms of a broken ankle can be feeling a numb or tingling sensation and/or what is called “crepitus” or a feeling of bone grinding on bone when the ankle is manipulated. Beyond a bone sticking out of the flesh, the only way to know for sure if you have a broken ankle is to obtain an X-ray or bone scan. If the ankle is broken, these diagnostic tests will show that something is out of place. A CT scan or MRI may be ordered to determine the severity of the break. It is vital to see a podiatrist if you have injured your ankle as this professional can order the appropriate test and proceed to treat the fracture or whatever condition might be identified.
If you sustain an injury to your ankle and wonder whether it is broken or not, you should remain calm and assess your symptoms. A broken ankle is quite painful, especially when you try to move it or put weight on it. The ankle is usually swollen from blood or fluid accumulating at the site of injury and it may be discolored or bruised. Less common symptoms of a broken ankle can be feeling a numb or tingling sensation and/or what is called “crepitus” or a feeling of bone grinding on bone when the ankle is manipulated. Beyond a bone sticking out of the flesh, the only way to know for sure if you have a broken ankle is to obtain an X-ray or bone scan. If the ankle is broken, these diagnostic tests will show that something is out of place. A CT scan or MRI may be ordered to determine the severity of the break. It is vital to see a podiatrist if you have injured your ankle as this professional can order the appropriate test and proceed to treat the fracture or whatever condition might be identified.
Broken ankles need immediate treatment. If you are seeking treatment, contact Joe Mathew George DPM, FACFAS from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Ankles
A broken ankle is experienced when a person fractures their tibia or fibula in the lower leg and ankle area. Both of these bones are attached at the bottom of the leg and combine to form what we know to be our ankle.
When a physician is referring to a break of the ankle, he or she is usually referring to a break in the area where the tibia and fibula are joined to create our ankle joint. Ankles are more prone to fractures because the ankle is an area that suffers a lot of pressure and stress. There are some obvious signs when a person experiences a fractured ankle, and the following symptoms may be present.
Symptoms of a Fractured Ankle
- Excessive pain when the area is touched or when any pressure is placed on the ankle
- Swelling around the area
- Bruising of the area
- Area appears to be deformed
If you suspect an ankle fracture, it is recommended to seek treatment as soon as possible. The sooner you have your podiatrist diagnose the fracture, the quicker you’ll be on the way towards recovery.
If you have any questions, please feel free to contact our offices located in Joliet, Bolingbrook, and Channahon, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
All About Broken Ankle
Broken ankles or “ankle fractures” are injuries that occur when the bones that make up the ankle joint are broken. Ankle injuries are some of the most common bone and joint injuries. The ankle joint is made up of three bones that join. The tibia is the main bone, and it makes up the inside of the anklebone. The fibula is a smaller bone, and it makes up the outside of the anklebone. A membrane called the joint capsule is lined with a layer called the synovium, which covers the entire joint. The synovium produces synovial fluid which allows for the joint surfaces to move.
An ankle becomes broken when the joint is stressed beyond the strength of its limits. When an ankle is fractured, ligaments may also tear at the same time. Fractures often occur to the ankle rolling or twisting in an unusual way. At times, a fracture may even be caused by an extreme force applied to the joint.
Symptoms of a broken ankle include pain, swelling, bruising, discoloration, numbness, and an inability to move the toes. If you have a broken ankle, you may also hear something tear or snap when you initially suffered the injury. If you have pain from a broken ankle, beware that the pain will not always come from the exact area of the fracture; you may also experience pain from associated foot fractures. The swelling you may experience can suggest that soft tissue damage may have occurred due to the injury.
There are differences between an ankle fracture and an ankle sprain. The difference is that a fracture or break in the bone is required to classify an injury as a broken ankle. An ankle sprain occurs when there is a tear or disruption of ligaments in the ankle. In some cases, the prognosis of an ankle sprain may be worse than that of a fracture.
X-rays are the most common way to diagnose a broken ankle. X-rays show if the ankle is broken and where exactly the fracture is located. It will also show how many pieces of broken bone there are. A second method of testing to see if an ankle is broken is a stress test. To do this, the doctor will put pressure on the ankle and perform a stress test to determine if the fracture requires surgery. Other methods for diagnosis include CT scans and MRI scans.
If you are suffering from a broken ankle, consult with your podiatrist immediately to receive a proper diagnosis and treatment.
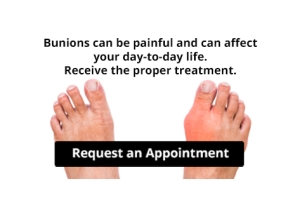
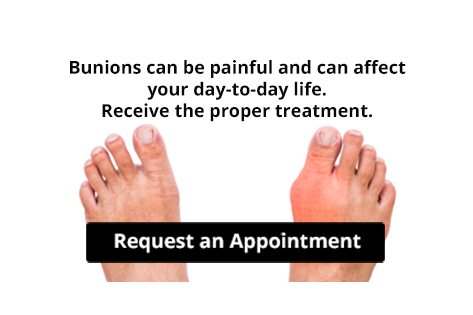
Are Bunions Affecting Your Everyday Life?
The Danger of Diabetic Foot Ulcers
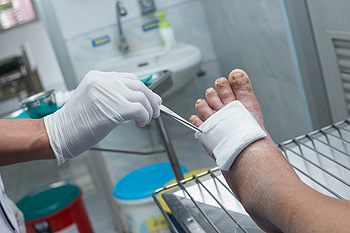
Some diabetic patients, roughly 15 percent, develop what is known as foot ulcers. The main cause is that their feet become numb, and they may not notice sores or open wounds on the bottom of their feet. When these sores fail to heal properly or become infected, they can lead to severe consequences, including amputation. Risk factors include smoking, insulin dependence, weight problems, ill-fitting footwear, high cholesterol and poor hygiene. Symptoms of diabetic foot ulcers are discoloration of toes and toenails, pain and redness, blisters, sores, calluses, pus or fluid discharge, and foul odor emanating from the feet. If diabetic foot ulcers have developed on your feet, it is suggested that you make an appointment with a podiatrist as soon as possible for an examination and ongoing treatment plan.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Joe Mathew George DPM, FACFAS from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Joliet, Bolingbrook, and Channahon, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
Dealing with Corns
Corns can sometimes be confused with calluses if you don’t know what to look (and feel) for. Corns can be painful and are either hard or soft. Hard corns, the most common type of corn, are caused by repeated pressure or friction. Soft corns are typically lighter in color and rubbery in texture. They usually form between toes. The best way to prevent corns from developing is to wear shoes that fit well and don’t cause pressure or friction on any part of your feet. Keep your toenails trimmed—but not so short that they grow into surrounding skin. Moisturize your feet daily and avoid wearing shoes without socks. People with diabetes, skin disorders or circulation problems would be wise not attempt to remove corns themselves, as such home remedies can sometimes lead to bleeding and infection. For safe and effective treatment for painful corns, it's a good idea to make an appointment with a podiatrist. They can also offer more tips and techniques for avoiding corns from developing in the first place.
If you have any concerns regarding your feet and ankles, contact Joe Mathew George DPM, FACFAS of Illinois. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our offices located in Joliet, Bolingbrook, and Channahon, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.